In 2022, Sanger, Texas mom Nikki Johnson was having a textbook pregnancy. COVID restrictions meant that her husband, Devon, wasn’t able to make all her appointments, but overall, everything seemed ready for a scheduled induction at 39 weeks. They had decided early in the pregnancy to let the gender of the baby be a surprise, so they eagerly awaited meeting their son or daughter. Then, things took an unexpected turn during labor.
“I remember turning to the nurses and asking, ‘Is this normal? I feel like I’m going to black out,’” Nikki recalls. Her world went dark.
The next parts of her pregnancy have been pieced together by her husband’s words and medical records. Nikki had experienced a very rare pregnancy complication called an amniotic fluid embolism (AFE), an allergic-like reaction to amniotic fluid entering the mother’s bloodstream, which is usually a normal part of childbirth. For Nikki, it led to respiratory failure.
This rare birth complication is unpredictable, unpreventable and only happens roughly 1 in 40,000 births. (To put that into perspective, it equates to approximately 100 times a year in the United States out of 4 million births.)
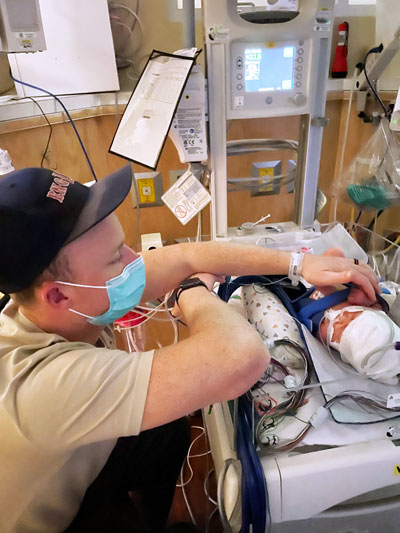
Treatment for AFE requires blood product—and Nikki received over 31 units during her nine-day stay in the intensive care unit (ICU) and in the mother and baby unit. Her baby girl was airlifted to a separate hospital that could care for her needs in a high-level neonatal intensive care unit (NICU).
“I had amazing care from the doctors to the nurses, and even hospital administrators making sure my family and I were provided for, despite COVID restrictions,” said Nikki. “But no matter how wonderful the care I received was, I would not be alive today without blood donations.”
Through the work of the Amniotic Fluid Embolism Foundation, Nikki was introduced to the team at MoMMA’s Voices, a maternal health patient advocacy coalition established in 2018 and comprised of over 20 maternal health organizations that work to amplify the voices of those who have experienced pregnancy and childbirth complications or loss.
MoMMA’s Voices’ goal is to equip and activate patients and family members as partners with healthcare providers and researchers who are working to improve maternal health outcomes. Nikki had healthcare providers who knew exactly what actions to take to save the lives of her and her baby—but that’s not the case for all women in the United States.
“In 2021, we lost 1,200 mothers in the U.S. to pregnancy-related causes, which is more than most every other country in the developed world,” said MoMMA’s Voices Program Director Nicole Purnell. “We know that the only way to decrease those numbers is to help mommas to be heard and integrated into improving how pregnancy and postpartum care is provided in the U.S.”
Nikki wanted to share her experience to raise awareness of AFE and to draw attention to the role of blood donations in saving the lives of moms and babies. She decided to participate in a specialized training program provided by MoMMA’s Voices called the Patient Family Partner certification.
Getting Trained to Create Maternal Health Change
The Patient Family Partner (PFP) training program is a set of online, self-paced training modules that help women and family members who have gone through a difficult pregnancy experience to become advocates. The training includes content on advocate readiness, how to tell your story, and building your resume as a trained advocate.
Any woman who has experienced a complication like high blood pressure or preeclampsia, hemorrhage, premature delivery, placenta accreta, AFE, maternal mental health disorders like postpartum depression or postpartum anxiety, or other issues is welcome to participate in the training.
Once a person completes the PFP training, they are matched together with opportunities to serve as patient representatives on maternal health quality improvement initiatives.
“Texas is leading the way for groundbreaking healthcare practices in prenatal care, working hard to ensure that hundreds of hospitals provide top-of-the line treatments,” said Purnell. “But we need more people joining us and sharing their lived experience to truly implement change.”
The MoMMA’s Voices team recently partnered with Texas state leadership to implement a large-scale program focused on improving outcomes due to hypertensive disorders of pregnancy. Over the next year, the program will have dozens of opportunities to join advisory councils and work with quality assurance professionals on Texas-focused initiative.
Contact MoMMA’s Voices to See How You Can Help
Are you a Texas mom who has faced pregnancy-related issues such as high blood pressure, infection, and excessive bleeding? You are not alone. The MoMMA’s Voices program would love to hear from YOU! Learn more at mommasvoices.org/texaspreeclampsia or by contacting them via email or social media.
Photos courtesy of Denton County and Nikki Johnson. Sponsored content for MoMMA’s Voices.